HPTN 094/ INTEGRA
HPTN 096
HIV Testing for Advocates
This slide deck provides and overview of HIV testing—types of test, WHO guidelines, current issues in testing, looking ahead, resources and more.
New Report: HIV Prevention R&D funding drops again
Today, we and partners are proud to release the annual HIV Prevention Research and Development Investments Report, with important findings for our collective advocacy. The report reveals a growing mismatch between the current promise of HIV prevention R&D, and continuing declines in the funding available. This decline affects both funding for research on new interventions and funding to expand access to existing prevention tools. The new report is based on outreach to 215 funders of HIV prevention R&D in the public, philanthropic and commercial sectors and includes 2020 funding data.
The latest data shows funding for HIV prevention R&D dropped by US$54 million (4.4 percent) in 2020. This second consecutive annual decrease is part of an eight-year trend of flat or declining funding for HIV prevention R&D.
The report also finds that financial support for HIV prevention R&D is almost entirely dependent on public sector funders, notably from the United States, and on one key United States-based philanthropic funder, the Bill & Melinda Gates Foundation. Commercial sector funding, already extremely low, dropped again in this year’s survey.
“These concerning trends in funding come at a promising but very demanding moment in efforts to control the pandemic,” said Mitchell Warren, executive director of AVAC, which coordinates the Resource Working Group with the International AIDS Vaccine Initiative (IAVI) and the Joint United Nations Programme on HIV/AIDS (UNAIDS). “Funding is declining just as the field confronts a new generation of opportunities and challenges.”
This high stakes environment includes: new products readying for introduction, such as injectable cabotegravir for PrEP and the Dapivirine Vaginal Ring; international support for ambitious new global targets for ending the epidemic; initial proof of concept of antibody-based prevention; and urgently needed new thinking for HIV vaccine development as recent trials have experienced setbacks and new technologies such as mRNA succeed against COVID-19.
Key findings from the report include:
HIV prevention R&D is highly overdependent on a few key funders, and much of the world is not contributing at the levels seen in prior years:
- HIV prevention R&D funding relies almost exclusively on the public sector, particularly the US public sector. The trend toward an overdependence on a small number of large investors, which the Working Group has surfaced and cautioned against in the past, intensified further in 2020.
- Globally, the public sector accounts for 86 percent of prevention R&D funding, with 92 percent of that coming from the US public sector.
- European public sector investments represent only 7 percent of the global total. While European public sector investment increased by 57 percent in 2020, it is still barely half of the US$124 million the European public sector contributed in 2009.
- The entire rest of the world accounted for only US$14 million, or just 1 percent of total public sector funding.
- Philanthropic funding, consisting almost exclusively of funding from the Bill & Melinda Gates Foundation, declined 20 percent in 2020 to US$127 million or 12 percent of the total global investment.
- Reported commercial sector support for HIV prevention R&D, already the lowest segment of investment, fell by 55 percent to US$31 million, or just 3 percent of the total, in 2020. While total commercial investment may be underreported, trends over time from the data collected show commercial sector investments is, by far, the smallest piece of the funding pie for HIV prevention R&D.
Funding dropped in 2020 across a number of key segments, including:
Preventive vaccine R&D: With two large-scale HIV vaccine trials underway, and dozens of new approaches under investigation, funding for preventive HIV vaccine R&D decreased by 5.5 percent or US$46 million in 2020 to US$802 million. While different European countries have increased or decreased their investments, overall European public sector investment in HIV vaccine R&D decreased 31 percent in 2020, to US$48 million.
R&D for PrEP, including pills, implants, injections: While uptake of oral PrEP grew substantially in 2020, and multiple recent research studies have demonstrated the potential impact of a range of PrEP options including long-acting injections, pills and implants, global investment in PrEP R&D declined 2 percent in 2020 to US$107 million. While US public sector donors increased funding for PrEP R&D by 5 percent, and commercial sector investment increased by 21 percent to US$24 million, neither was enough to overcome a 42 percent decline in funding from the philanthropic sector.
Voluntary Medical Male Circumcision (VMMC): As a number of studies affirmed the efficacy of VMMC over a decade ago, funding in the field is focused on implementation science, behavioral studies and advocacy and policy, each of which is vital to extending the reach and impact of this highly effective prevention tool. Yet investment in VMMC decreased by 37 percent to just US$6 million in 2020, almost all of which came from a single donor, the Bill & Melinda Gates Foundation.
Preventing vertical transmission: Prevention of mother-to-child transmission of HIV (PMTCT) remains a key prevention priority, but funding for PMTCT R&D decreased by 29 percent in 2020, from US$35 million to US$25 million. The decline is attributed to the loss of the Bill & Melinda Gates Foundation from the list of PMTCT R&D funders, and to decreases in funding from public donors. US public sector funding for PMTCT R&D fell 22 percent to US$22 million in 2020. European funding also fell more than 60 percent, from US$3.4 million in 2019 to US$1.3 million in 2020.
Only two areas of prevention R&D funding showed small increases in funding, including:
Treatment as Prevention (TasP): Long neglected in HIV prevention investment, funding for treatment as prevention (TasP) R&D increased from $1.7million to US$9 million in 2020. The increase came from philanthropy, notably the Bill & Melinda Gates Foundation (US$5 million) and the Wellcome Trust (US$1 million).
While TasP R&D funding is small overall, this increase is a hopeful sign that TasP may once again receive its appropriate focus as priority for HIV prevention research.
Microbicides: After multiple years of decline, investment in microbicide R&D registered a very small increase (0.4 percent or US$0.6 million) to US$145 million in 2020. Concerningly, there is even less diversity in microbicide funding than in HIV prevention R&D overall, with the public sector providing 99 percent of microbicide R&D resources.
While this tiny increase is a hopeful sign, it does not match the scope of the promise of microbicides. One key product, the Dapivirine Vaginal Ring, is now recommended by the WHO as an additional HIV prevention option. In addition, a range of promising microbicide strategies are under investigation. One, a 90-day dual-purpose vaginal ring designed to confer both contraceptive and HIV protection, was found to be effective in early testing.
This is the 16th annual report from the Resource Tracking for HIV Prevention Research & Development Working Group. Go to HIVResourceTracking.org to explore the key findings, funding trends, and previous reports in depth and follow the conversation on Twitter #HIVResearchFunding.
Press Release
HIV Prevention R&D Funding Drops Again, Even as Major Scientific Advances Require Support
A Worrying Trend Toward Overreliance on a Few Funders Increased in 2020
Contact
Kay Marshall, +1 (347) 249-6375, [email protected]
December 8, 2021 – The annual HIV Prevention Research and Development Investments Report reveals a growing mismatch between the current promise of HIV prevention R&D, and consistent declines in the funding available to both research new HIV prevention approaches and expand access to the prevention tools available today. The 2020 report, based on outreach to 215 funders of HIV prevention R&D in the public, philanthropic and commercial sectors, is the 16th annual report from the Resource Tracking for HIV Prevention Research & Development Working Group.
According to this year’s report, funding for HIV prevention R&D dropped by US$54 million (4.4 percent) in 2020. This second consecutive annual decrease is part of an eight-year trend of flat or declining funding for HIV prevention R&D. The report also finds that financial support for HIV prevention R&D is almost entirely dependent on public sector funders, notably from the United States, and on one key United States-based philanthropic funder, the Bill & Melinda Gates Foundation. Commercial sector funding, already extremely low, dropped again in this year’s survey.
“These concerning trends in funding come at a promising but very demanding moment in efforts to control the pandemic,” said Mitchell Warren, executive director of AVAC, which coordinates the Resource Working Group with the International AIDS Vaccine Initiative (IAVI) and the Joint United Nations Programme on HIV/AIDS (UNAIDS). “Funding is declining just as the field confronts a new generation of opportunities and challenges. These include the introduction of injectable cabotegravir for PrEP and the Dapivirine Vaginal Ring, ambitious new global targets for ending the epidemic, initial proof of concept of antibody-based prevention, and the need to rethink HIV vaccine development in light of setbacks in recent trials and the possible promise of mRNA and other vaccine approaches.”
Among the key findings from the annual HIV Prevention Research and Development Investments Report are the following:
HIV prevention R&D is highly overdependent on a few key funders, and much of the world is not contributing at the levels seen in prior years.
- HIV prevention R&D funding relies almost exclusively on the public sector, particularly the US public sector. The trend toward an overdependence on a small number of large investors, which the Working Group has surfaced and cautioned against in the past, intensified further in 2020.
- Globally, the public sector accounts for 86 percent of prevention R&D funding, with 92 percent of that coming from the US public sector.
- European public sector investments represent only 7 percent of the global total. While European public sector investment increased by 57 percent in 2020, it is still barely half of the US$124 million the European public sector contributed in 2009.
- The entire rest of the world accounted for only US$14 million, or just 1 percent of total public sector funding.
- Philanthropic funding, consisting almost exclusively of funding from the Bill & Melinda Gates Foundation, declined 20 percent in 2020 to US$127 million or 12 percent of the total global investment.
- Reported commercial sector support for HIV prevention R&D, already the lowest segment of investment, fell by 55 percent to US$31 million, or just 3 percent of the total, in 2020. While total commercial investment may be underreported, it is still the smallest piece of the HIV prevention R&D funding pie.
Funding dropped in 2020 across a number of key HIV prevention R&D segments, including:
Preventive vaccine R&D: With two large-scale HIV vaccine trials underway, and dozens of new approaches under investigation, funding for preventive HIV vaccine R&D decreased by 5.5 percent or US$46 million in 2020 to US$802 million. While different European countries have increased or decreased their investments, overall European public sector investment in HIV vaccine R&D decreased 31 percent in 2020, to US$48 million.
R&D for PrEP, including pills, implants and injections: While uptake of oral PrEP grew substantially in 2020, and multiple recent research studies have demonstrated the potential impact of PrEP in the form of long-acting injections, pills, implants and rings, global investment in PrEP R&D declined 2 percent in 2020 to US$107 million. While US public sector donors increased funding for PrEP R&D by 5 percent, and commercial sector investment increased by 21 percent to US$24 million, neither was enough to overcome a 42 percent decline in funding from the philanthropic sector.
Voluntary Medical Male Circumcision (VMMC): As a number of studies affirmed the efficacy of VMMC over a decade ago, funding in the field is focused on implementation science, behavioral studies and advocacy and policy, each of which is vital to extending the reach and impact of this highly effective prevention tool. Yet investment in VMMC decreased by 37 percent to just US$6 million in 2020, almost all of which came from a single donor, the Bill & Melinda Gates Foundation.
Preventing vertical transmission: Prevention of mother-to-child transmission of HIV (PMTCT) remains a key prevention priority, but funding for PMTCT R&D decreased by 29 percent in 2020, from US$35 million to US$25 million. The decline is attributed to the loss of the Bill & Melinda Gates Foundation from the list of PMTCT R&D funders, and to decreases in funding from public donors. US public sector funding for PMTCT R&D fell 22 percent to US$22 million in 2020. European funding also fell more than 60 percent, from US$3.4 million in 2019 to US$1.3 million in 2020.
Only two areas of prevention R&D funding showed small increases in funding, including:
Treatment as Prevention (TasP): Long neglected in HIV prevention investment, funding for TasP R&D increased from $1.7million to US$9 million in 2020. The increase came from philanthropy, notably the Bill & Melinda Gates Foundation (US$5 million) and the Wellcome Trust (US$1 million).
While TasP R&D funding is small overall, this increase is a hopeful sign that TasP may once again receive its appropriate focus as priority for HIV prevention research.
Microbicides: After multiple years of decline, investment in microbicide R&D registered a very small increase (0.4 percent or US$ 0.6 million) to US$145 million in 2020. Concerningly, there is even less diversity in microbicide funding than in HIV prevention R&D overall, with the public sector providing 99 percent of microbicide R&D resources.
While this tiny increase is a hopeful sign, it does not match the scope of the promise of this approach. One key product, the Dapivirine Vaginal Ring, is now recommended by the WHO as an additional HIV prevention option. In addition, a range of promising microbicide strategies are under investigation. One, a 90-day dual-purpose vaginal ring designed to confer both contraceptive and HIV protection, was found to be effective in early testing.
Pandemic preparedness requires greater investment in HIV, other current health crises
“The response to the COVID-19 pandemic has demonstrated that when there’s political will, global solidarity, and significant financial investments, rapid developments of new prevention technologies such as vaccines happen,” said Shannon Hader, deputy executive director of programme, UNAIDS. “This is the time to mobilize investments in HIV service delivery/prevention research and galvanize momentum to achieve the broader 2025 AIDS targets.”
Methodology: HIV prevention R&D investment figures are collected annually by the Resource Tracking for HIV Prevention R&D Working Group through an email survey. For the present report, the Working Group reached out from February to June 2020 to 215 funders in the public, philanthropic and commercial sectors. Two different types of resource flows were tracked: investments, defined as annual disbursements by funders; and, when available, expenditures, defined as resources directly spent on R&D activities by funding recipients. More information about the report methodology is at www.hivresourcetracking.org/about/methodology.
###
About the Resource Tracking Working Group: In its 16th annual report, the Resource Tracking for HIV Prevention Research & Development Working Group (“Working Group”) documents research and development spending for the calendar year 2020 and analyzes funding trends spanning twenty years. The Working Group is led by AVAC in partnership with the International AIDS Vaccine Initiative and UNAIDS.
Undetectable = Untransmittable Resources
This website from the Prevention Access Campaign is filled with links to the latest information on Undetectable = Untransmittable as well as other pertinent documents and resources.
IAS 2021: Our take and updates
COVID-19 may have forced some limiting factors onto the 11th IAS Conference on HIV Science—the conference was primarily online; the attendance was lower; and we couldn’t interact with our colleagues face-to-face—but moving in and out of virtual sessions, something transformative was in the air. The intersection of the responses to COVID-19 and HIV and the glaring disparities in health made ever more undeniable by COVID-19, are giving new meaning and momentum to changes advocates have been pressing for years, even decades. Where to begin…
- DSD: The time is now
- The latest on the prevention pipeline
- And vaccines?
- COVID-19 and HIV
- PrEP and resistance
- Calls for people-centered solutions
- New targets, old problems
DSD: The time is now
Differentiated service delivery (DSD) accelerated by orders of magnitude—telephone counseling, dispensing multi-month supplies of drugs, home delivery, community-based refills, and other innovation staved off hundreds of thousands of predicted HIV deaths, which were expected if people couldn’t get to the pharmacy or the clinic for treatment during COVID-19 lockdowns.
Multiple conference sessions referred to numerous initiatives where DSD scaled up rapidly, and with success. A few examples: An initiative from the CQUIN network coordinated among 21 different countries to share resources and lessons on DSD. PEPFAR’s Catherine Godfrey reported from a review of 52 countries that found 30 of them had scaled up and expanded eligibility for multi-month dispensing for treatment, with a 79 percent increase in the total number of people receiving a six-month supply of drugs. A different review from seven PEPFAR-supported countries, showed overall treatment interruption did not increase. And a UNAIDS analysis showed global trends in ART initiation continued despite the lockdown. Crucial to these successes, said Godfrey, were community health workers and community-based drug distribution.
These lessons from antiretroviral treatment have been applied in prevention as well. The session, Paving the road for new PrEP products: The promise of differentiated, simplified, and decentralized delivery to maximize the potential of new products, expanded the discussion on the need for innovations in PrEP delivery. Panelists at the satellite session, convened by AVAC, IAS and PATH, noted delivery must evolve as new products move through the pipeline, or years will be wasted with low uptake. Simplifying and Improving PrEP Delivery is one of four issue briefs just published by the Prevention Market Manager project and launched at the satellite, along with Reframing Risk in the Context of PrEP, Generating and Sustaining Demand for PrEP, and Next Generation M&E for Next-Generation PrEP. All echo core principles embedded in DSD: center the development of programs, policies and products in the leadership and knowledge of those who need prevention most.
This movement to DSD holds tremendous potential for prevention just as the field is poised to add powerful new prevention options to the tool kit. Data on next-generation options were also presented at IAS.
The latest on the prevention pipeline
Days before IAS began, The HealthTimes reported Zimbabwe’s approval of the monthly Dapivirine Vaginal Ring (DVR), which would be the first country to do so. Data presented at IAS on ring use from the REACH study underscore what can be achieved by tailoring the design of products and programs. REACH is a study looking at safety and adherence of oral PrEP and the ring in young women ages 16-21. Data from the study showed a marked increase in adherence to both the ring and oral PrEP among adolescent girls compared to previous studies. The key factor in the uptick? Intensive, individualized support that allowed participants to select from a menu that included text messages, weekly check-ins by phone, “peer-buddy” and adherence support groups. These findings build on evidence from other studies, including the POWER study, that adolescents greatly benefit from intensive adherence support. REACH data on preferences between the ring and oral PrEP are forthcoming.
A ring-focused session—Intravaginal options: Today and in the future—covered a lot of ground, from early-stage research on multipurpose rings for prevention, to work the World Health Organization (WHO) is doing to help facilitate the introduction of the Dapivirine Vaginal Ring. The WHO already recommends the ring and its Coordinator of Treatment and Care in the Department of HIV/AIDS, Meg Doherty, said the WHO plans to develop tools and guidance to assist countries to fit this new tool into their context, work on the supply chain, generate demand and more. These tools and guidance are expected by early 2022.
On the research front, Andrea Thurman (CONRAD) presented data from Phase I studies of a ring loaded with levonorgestrel (LNG) and tenofovir (TFV) and showed it is safe, acceptable and met benchmarks for drug levels in the body. Further research is warranted. Another presentation in that session came from Sharon Hillier (UPMC Magee-Womens Hospital), who presented highlights from the pipeline of intravaginal ring research including a three-month Dapivirine Ring and a novel MPT ring that’s both non-hormonal and includes a non-ARV-based antiviral.
A satellite session, Bringing the Dual Prevention Pill to Market: Opportunities for HIV and Pregnancy Prevention and Implications for Future Multipurpose Prevention Technologies (MPTs), reviewed the status of the Dual Prevention Pill, which could be available as early as 2024. If approved, it would be the first MPT to go to market since male and female condoms. This novel strategy provides unprecedented opportunities to integrate sexual and reproductive health (SRH) with HIV services, but major challenges must be met. The field of women’s health and family planning, policy makers and all stakeholders will need to understand why and how HIV prevention is their priority too, and how the DPP fits in the context of community health. Early, frequent and comprehensive consultations across both fields can and must serve as a model for breaking down these silos.
In a late-breaker session, Sharon Hiller presented data from the Phase 2a study of monthly oral islatravir, building on data presented earlier this year at HIVR4P. Hillier’s presentation at IAS 2021 showed this strategy met—and exceeded—key benchmarks for drug levels in the body that researchers think will be needed for it to be effective. The week-24 data also showed that it’s safe and well-tolerated. Efficacy data on this new prevention option will come from two large-scale efficacy trials (IMPOWER-22 and IMPOWER-24), results of which are expected in 2024. Islatravir is also being studied for long-term use via an implant.
And vaccines?
With a robust non-vaccine prevention pipeline, some of the vaccine session titles seemed to hint at a field wondering about its place: Will there be a next generation HIV vaccine if current ones fail?; An HIV vaccine: who needs it?; and HIV vaccines and immunotherapy: Quo vadis? (Latin for “Where are you going?”) The answer to that question is that HIV vaccine research is moving forward. Discussions at these sessions pointed to intensifying global interest in vaccine research and implementation, with COVID on everyone’s mind—and much of the success in COVID vaccines owed to the legacy of research in HIV. HIV vaccine research is moving forward with diverse approaches, and efficacy data from the two ongoing large-scale trials of Janssen’s Adeno 26-based vaccine are expected within the next two years. The AMP trials, and their implications for vaccine and antibody research, were also part of the discussion and are discussed in more detail in our recent document, Understanding Results of the AMP Trials.
But this momentum can’t be taken for granted. As Lynn Morris, from the University of the Witwatersrand and a leading antibody researcher, said in her plenary, it’s important now to galvanize political will, support increased investment and industry involvement in HIV vaccine development, run more parallel trials and take more risk.
And no matter the challenges of vaccine science, once available people will need to take it. AVAC’s Daisy Ouya reminded attendees at a UNAIDS/HIV Vaccine Enterprise satellite session that early and consistent community engagement is essential. If the field is going to reach coverage targets, community mistrust can’t be a barrier.
COVID-19 and HIV
A WHO report found HIV is a risk factor for severe or critical COVID-19. The WHO Global Clinical Platform for COVID-19 drew data from 24 countries and more than 15,000 people. This report offers another picture on HIV and COVID from the largest pool of data to date compared to other smaller studies that did not find a link, including one from the US, also presented at IAS 2021. The results have reinforced the need to ensure people living with HIV are listed as priority populations to receive COVID vaccines across the globe. This must happen in the context of massive scale-up to produce and distribute vaccines and close the gap in vaccination between the global north and south.
PrEP and resistance
The GEMS project monitored for the development of drug resistance among PrEP-takers. The project analyzed samples from 104,000 people from PrEP programs in Eswatini, Kenya, South Africa and Zimbabwe. There were 229 documented seroconversions overall and 118 were sequenced (some participants didn’t provide samples and some samples had low viral load and couldn’t be sequenced). Of those 118, 23 percent had HIV with a PrEP-associated mutation for drug resistance. Urvi Parikh, Senior Project Advisor of GEMS, presented the data and put the findings in context: the number of reported infections while on PrEP was very small, and an even smaller number had resistant mutations.
Based on the GEMS data, the most common mutation, M184V/I, is not expected to undermine the efficacy of one of the most important treatments across Africa, dolutegravir-based regimens. It will be important to monitor where these mutations will affect future treatment. It will also be vital to carefully screen for HIV among people who want PrEP in order to catch early infections that could lead to resistance. For additional background, our colleague Gus Cairns did a terrific summary of these findings as part of the NAM/AIDSMAP reports throughout the conference.
Calls for people-centered solutions
IAS 2021 heard an emphasis on the importance of community-led, client-controlled empowerment and leadership, which starts at the beginning of the research process, framing the questions that must be answered and how to answer them.
No Data No More: Manifesto to Align HIV Prevention Research with Trans and Gender Diverse Realities launched during IAS 2021. Developed by trans and gender-diverse (TGD) advocates from South Africa, Europe and the United States, with support and solidarity from AVAC, the manifesto demands an HIV prevention research agenda based on the priorities of TGD communities, with those communities driving decisions throughout the process.
Among the demands: provide gender-affirming hormone treatment (GAHT) across the continuum of HIV research, prevention and care; address the barriers that limit access to research and prevention for TGD people; recruit TGD researchers and other experts to design and implement solutions at all phases of the response.
At a session, What is missing in the HIV response?: Strengthening HIV programmes for trans populations in the Global South, presenters decried the absence of data on trans health outcomes even as TGD people face high risk of HIV. See US CDC statistics that show 1 in 7 (14 percent) transgender women in the United States have HIV and an estimated 3 percent of transgender men have HIV, with even less data available for non-binary individuals.
Liberty Matthyse of Gender Dynamix in South Africa said “trans and gender-diverse healthcare is greatly understudied,” fundamentally undermining the effort to end the epidemic. “We need to prioritize community-led participatory research, plug into existing community-led movements, co-create context-specific methodology to reach missing and undocumented cases. And we need to decentralize access to hormonal care and make it part of a package of HIV services. Every person should have the right to gender self-determination.”
Rena Janamnuaysook’s presentation at this session provided a model. At Thailand’s Tangerine Clinic, members of the trans community identified priority health needs, co-designed a program of services, and received training to deliver qualified care. About 4,000 community members rely on the clinic, which offers hormone services and other gender-affirming care as an anchor to generate demand for other health services including HIV testing, prevention and treatment. Nearly all (94 percent) of the 10 percent who have tested positive have initiated ART, nearly all of them (97 percent) are virally suppressed, and 18 percent of those who have tested negative initiated PrEP. “Key populations-led services increased access to testing, simplified services, and promoted a sustainable HIV response,” said Rena.
New targets old problems
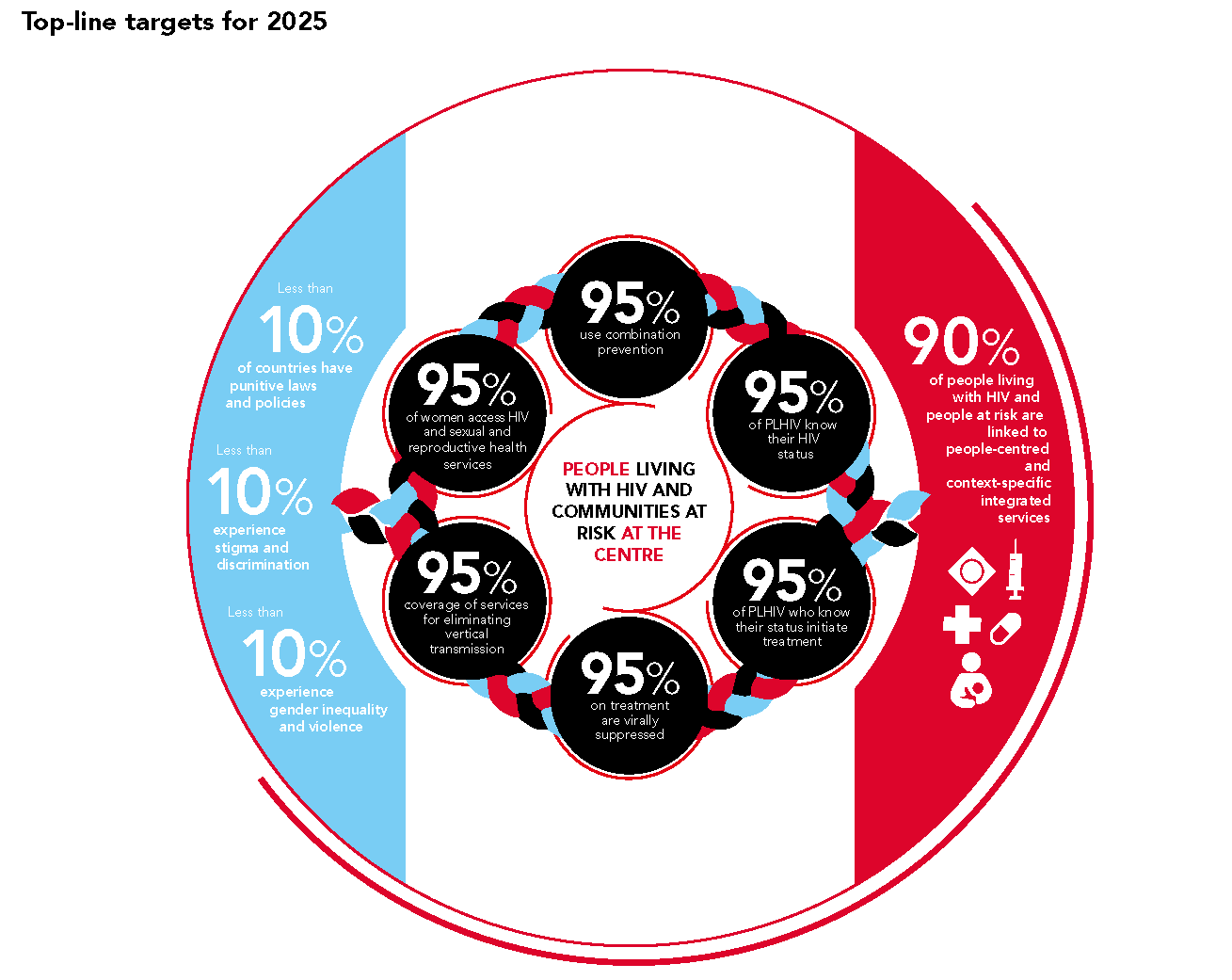
These stories from IAS 2021 put the past year in perspective. The science that was needed to respond to both SARS-CoV2 and HIV has seen significant advances and must continue. The innovation to deliver treatment and prevention has also seen unprecedented effort, and must accelerate and expand. But policy and political will has failed to close gaping inequities that mean, among other things, the 3.3 billion doses of COVID vaccine delivered to date are concentrated in a few wealthy countries, that lockdown drove up reports of rape in Uganda by 24 percent while the use of PEP dropped by 17 percent, that 150 million people will fall into extreme poverty this year, that COVID remains a threat to global health everywhere.
The new UNAIDS targets, the so called “10’s” aimed at social factors that drive epidemics (punitive laws and policies, stigma, discrimination and gender-based violence) should galvanize action from every quarter. Approved by the UN’s High Level Meeting on HIV in June, these new targets must be used to build on the sweeping changes underway in 2020, to dismantle structural barriers and to embrace new evidence-based models that will make prevention a reality everywhere it’s needed.
Research Literacy Zone Roundup
Alongside last week’s IAS 2021 Conference, AVAC and partners hosted a range of dynamic sessions in the virtual Research Literacy Zone, where researchers and advocates explored timely topics including: Dapivirine Vaginal Ring rollout, advances in vaccine and cure research, U=U, new approaches to understanding social factors that impact health, vaccine hesitancy and more. The Zone is a gathering place for researchers and community advocates to dive deep on critical topics in a small-scale environment.

All Zone sessions are available on our Research Literacy Zone page and on ENGAGE, AVAC’s online platform for peer-to-peer resource-sharing and collaborative learning. Register for your free account today, join the conversation, and access all that ENGAGE has to offer.
Also, the Zone isn’t just for conferences! AVAC hosts virtual events and conversations throughout the year (including an August 11 rectal microbicides webinar with AFC!). Have a topic idea for a future session? Drop us a note!
RESEARCH LITERACY ZONE @ IAS 2021
- HIV Cure Research in Africa: Challenges and Opportunities
- Pushing U=U Jigsaw Puzzle into the HIV Prevention Agenda
- Models, Maps and Measures: What advocates need to know about new strategies assessing social determinants
- A Conversation with Advocates on Vaccine Hesitancy
- Inclusion of Pregnant and Breastfeeding Women in HIV Prevention Research: What can you and I do to move this agenda forward
- Ring Roundup
HIV Cure Research in Africa: Challenges and opportunities included a panel of researchers and advocates exploring some of the challenges and opportunities of HIV cure research on the African continent, strategies that are currently being pursued, and the science of the cases of HIV cure reported in the news. Listen to the recording.
Pushing U=U Jigsaw Puzzle into the HIV Prevention Agenda focused on efforts to use the science of U=U to promote HIV treatment uptake, enhance adherence and eliminate stigma and discrimination, so that PLWHIV can live longer and have healthy relationships while protecting their partners from contracting HIV. Listen to the recording.
Models, Maps and Measures: What advocates need to know about new strategies assessing social determinants focused on how to assess the social determinants of HIV and a special NIH-funded initiative on the issue. The expanding pipeline for HIV prevention was one of the driving factors motivating the NIH to fund an initiative examining new ways of measuring social determinants.. The discussion focused on two new strategies: using models to determine what factors enhance the effectiveness of cash transfers in adolescent girls and young women in South Africa, and the use of GPS tracking to determine barriers to PrEP access in young MSM in NYC. Listen to the recording.
A Conversation with Advocates on Vaccine Hesitancy provided attendees a space to reflect on the urgent need for vaccine equity and potential vaccine hesitancy. Panel members discussed why some individuals are hesitant in their communities. The discussion also focused on solutions, with panel members and participants sharing what has worked in their contexts and resources they are developing to engage communities in the discussion now. Listen to the recording.
Inclusion of Pregnant and Breastfeeding Women in HIV Prevention Research: What can you and I do to move this agenda forward centered on the importance of including pregnant and breastfeeding women in HIV prevention trials. The discussion outlined barriers to participation and implementation and focused on steps to move the field forward. Listen to the recording.
Ring Roundup covered updates in the research program and rollout plans for the Dapivirine Vaginal Ring (DVR). Attendees learned about IPM’s DVR research program and the early-phase research pursuing a longer-acting formula and dual prevention (HIV and pregnancy). Discussion also focused on the current regulatory approval process of the ring as a prevention option for women and the steps advocates can take to secure national approvals. Listen to the recording.
Stay tuned for our full roundup of IAS conference news later this week, and remember, check out ENGAGE for future events and conversations, and let us know if you have an idea to share!
AVAC’s “3D” View of the World: 2019 and beyond
This infographic lays out AVAC’s top-line recommendations from AVAC Report 2019: Now What? The recommendations fall into three categories: deliver — prevention programs whose impact is well-measured and -defined; demonstrate — next-generation engagement for next-generation trials; develop — new targets for the post-2020 world.
UNAIDS Fast-Track Targets: The plan and the progress
The most widely-known UNAIDS Fast-Track goals were the 90-90-90 targets focused on diagnosing people with HIV, linking them to ART and supporting them to achieve virologic suppression. But these were only part of what the UNAIDS modelers said was needed to reduce new HIV diagnoses to 500,000 per year; the model also included significant scaling up of primary prevention including the targets listed below. There are gaps across the board, which helps explain how the world fell short of the hoped-for reduction in new HIV diagnoses.
Excerpted from AVAC Report 2019: Now What?